Acute provoked neonatal seizures (also known as acute symptomatic neonatal seizures) can occur in newborns whose brains are injured by a range of causes from stroke and bleeding in the brain to central nervous system infections. While the seizures themselves are scary enough for the families, the story continues after the neonates are treated for their initial seizures and discharged from the hospital; the children may continue to experience developmental challenges into childhood. However, when medical professionals are asked by concerned parents about the long-term prognosis for their children, the lack of sufficient data makes it difficult to give reassurance or recommendations. A new article published in Annals of Neurology aimed to address part of this challenge by providing data from children aged 5-6 who were enrolled in a multicenter study after experiencing acute seizures very early in their lives.
The authors conducted a statistical analysis of a subset of children enrolled in the Neonatal Seizure Registry (NSR) in order to look for patterns in the prevalence and potential causes of a number of developmental challenges. The NSR was co-founded by Renée A. Shellhaas, MD, MS, the David T. Blasingame Professor of Neurology at Washington University School of Medicine in St. Louis, and Hannah Glass, MD, MAS, of University of California, San Francisco. It has been enrolling patients across nine centers in the U.S. since 2012, with over 800 families and children evaluated, over 30 publications and seven completed or ongoing studies.

This study follows on two earlier NSR-based studies published by Shellhaas and colleagues. In the 2021 studies, newborns who experienced acute seizures and were enrolled at an NSR site were followed up to 24 months of age to understand whether antiseizure medicines should be continued after hospital discharge and what their likelihood of experiencing additional seizures or neurodevelopmental challenges may be. Results supported the safety of early discontinuation of antiseizure medications. However, there remained insufficient data on long-term outcomes in survivors of neonatal seizures, making it difficult for physicians to determine a customized follow-up care plan or counsel parents on how best to help their children. The NSR investigators have continued to collaborate closely with their parent advisory panel to address these knowledge gaps.
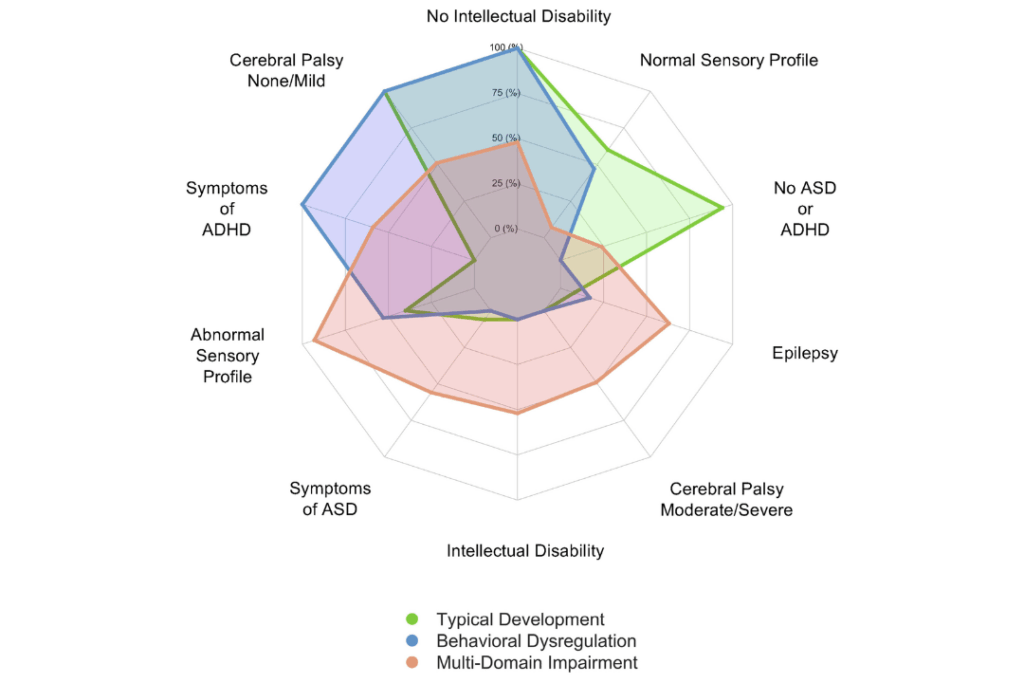
This 2026 follow-up study at the 5–6-year mark represents an important step forward in addressing the current gap in information. The researchers evaluated 144 children on a total of ten neurodevelopmental outcomes including epilepsy, cerebral palsy, attention-deficit/hyperactivity disorder (ADHD), autism spectrum disorder (ASD) and intellectual disability. Based on this evaluation, children were grouped into three categories: Multi-Domain Impairment, Behavioral Dysregulation and Typical Development.
Twenty-four percent of the 144 children evaluated in this study showed what the researchers classified as “multi-domain impairment,” with a high likelihood of epilepsy and moderate to severe impairment across cognitive, physical, behavioral and social domains. The vast majority of the children in this group required special supports as they entered school, such as individualized education or a 504 plan. A statistical analysis indicated that abnormal neonatal neurological examination at the time of hospital discharge, functional impairment during infancy on the Warner Initial Developmental Evaluation of Adaptive and Functional Skills and epilepsy at 12-24 months were statistically associated with a higher likelihood of being in the Multi-Domain Impairment group at age 5 to 6.
Thirteen percent of the children had otherwise normal development, with no cerebral palsy and very low risk for epilepsy, but had ADHD diagnoses or other test scores indicating hyperactivity or inattention. This indicates a clear need for behavioral and executive function screening at school entry for children who experienced acute seizures as newborns. The statistical analysis did not reveal any specific risk factors for being in the Behavioral Dysregulation group, making it all the more imperative to standardize behavioral screening for children who experienced neonatal seizures.
Finally, while 63% of the children were classified as showing typical development, 41% of the children in this group had abnormal sensory processing according to a validated sensory profile measure, meaning that they may have strong reactions to sensory inputs such as light or sound, become disruptive in the classroom or struggle to sit still. These types of difficulties can adversely impact a child’s school experiences, but can be addressed with relatively simple classroom modifications, indicating a need for sensory processing screening for children with a history of acute neonatal seizures as they prepare to enroll in school.
The main takeaway from the study is the importance of screenings, both behavioral and sensory processing, regardless of whether or not a child who experienced acute neonatal seizures has obvious developmental challenges. “Normal early development doesn’t tell the whole story after acute neonatal seizures,” said Shellhaas, who is senior associate dean for faculty promotions and career development at WashU Medicine. “Our data show that screening at school entry is critical—not optional—for these children.” Importantly, 82% of the children in the study who experienced acute seizures as newborns were in mainstream classrooms at age 5 to 6, which could provide some reassurance to parents whose babies have had such seizures, the researchers noted.
While this study makes an important contribution to the field’s understanding of long-term impacts of neonatal acute seizures, the authors emphasized the need for further research. Studies with larger sample sizes could help identify predictors of behavioral dysregulation, for instance, and longer-term studies would allow for more accurate risk prediction for developmental outcomes. Continuing to follow the current study cohort will also allow researchers to monitor the development of ADHD or ASD in the children as they get older and as the cognitive, social and behavioral demands they experience increase. Shellhaas, who served as senior author for this article as well as first or senior author for the two earlier articles, emphasized the need for continued studies of this group of children. “The path forward is clear,” she said. “We need systematic, longitudinal follow-up that extends well beyond the NICU.”
Glass, H.C., Numis, A.L., Soul, J.S., Wusthoff, C.J., Lemmon, M.E., Benedetti, G.M., Chu, C.J., Massey, S.L., Thomas, C., Anwar, T., Sturza, J., Berl, M.M., Li, Y., Rogers, E.E., Rau, S., Gidley Larson, J.C., Guerrero, J.L., Franck, L.S., McCulloch, C.E. and Shellhaas, R.A. (2026), Profiles and Predictors of Neurodevelopmental Outcome at 5–6 Years in Children With a History of Acute Provoked Neonatal Seizures. Ann Neurol. https://doi.org/10.1002/ana.78100